Life can feel UNBEARABLE
These Teddys have chronic pediatric cholestatic
liver disease—and it’s unbearable.
Learn more about their individual journeys with
Alagille syndrome and progressive familial
intrahepatic cholestasis (PFIC).
These Teddys have chronic pediatric cholestatic
liver disease—and it’s unbearable.
Learn more about their individual journeys with
Alagille syndrome and progressive familial
intrahepatic cholestasis (PFIC).
Cholestasis results from an impairment in bile formation or flow at some point between the liver cells, which produce bile, and the duodenum. When bile flow is stopped, bile acids build up in the liver. This can lead to a range of clinical presentations, from debilitating symptoms such as pruritus to liver injury to progressive liver disease, and, if left untreated, can result in fibrosis, cirrhosis, liver failure, and death. In addition, there is spillover of bile into the bloodstream, resulting in increased serum bile acids (sBA).1,2
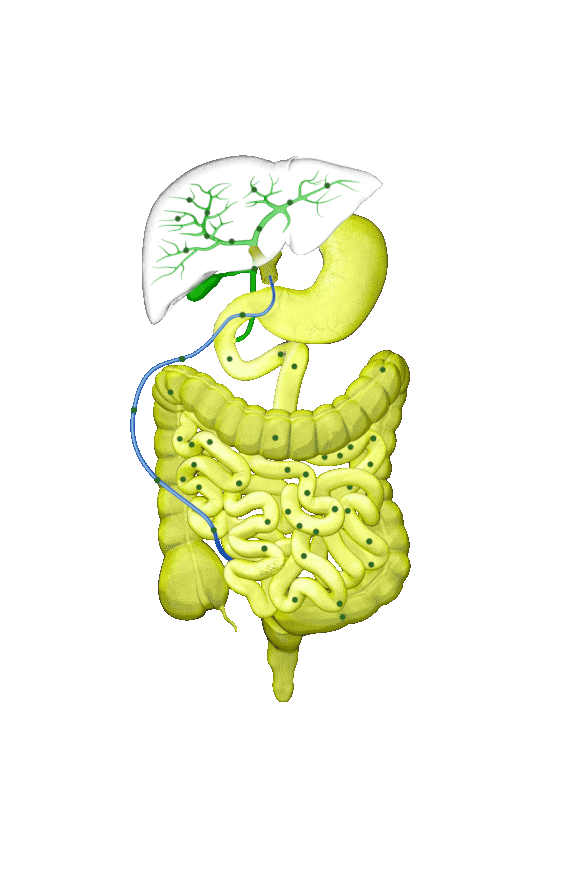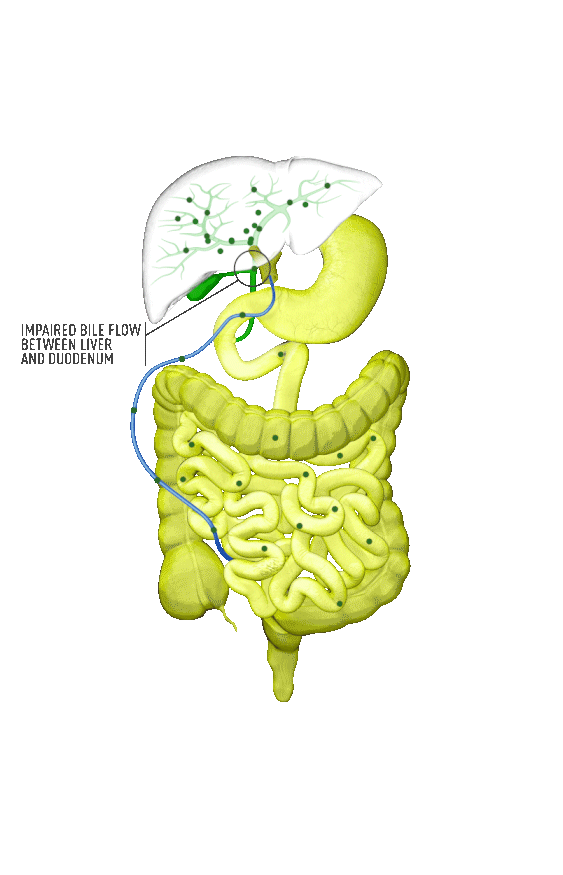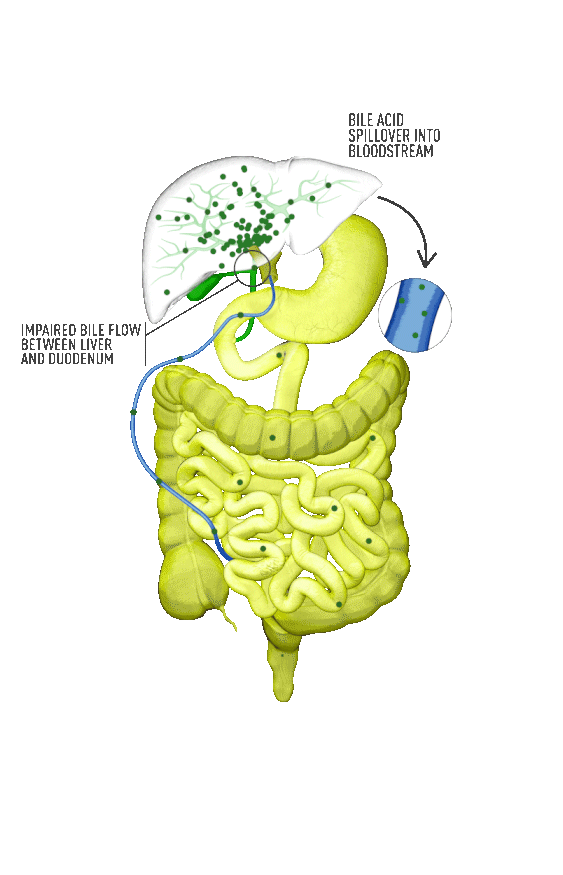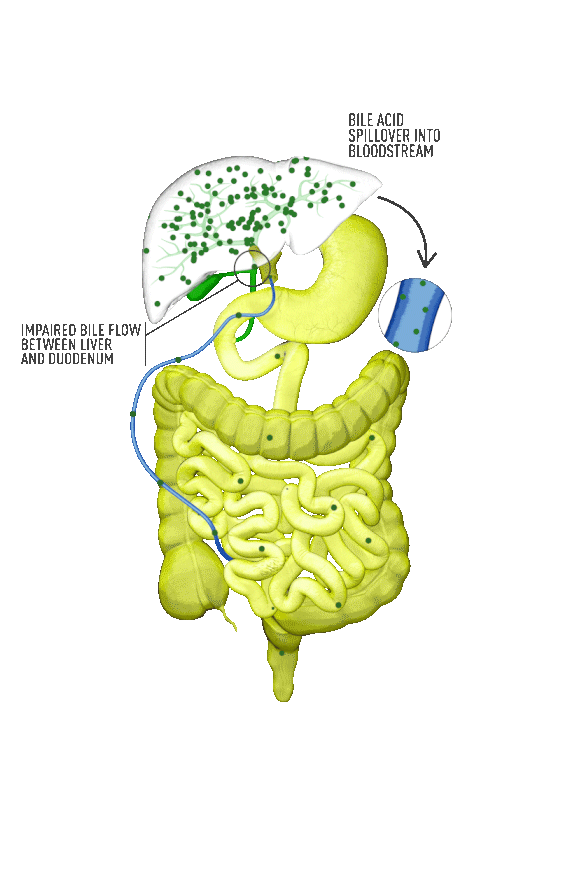
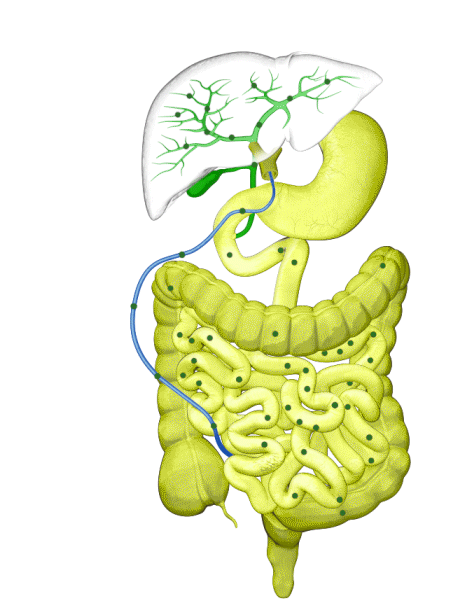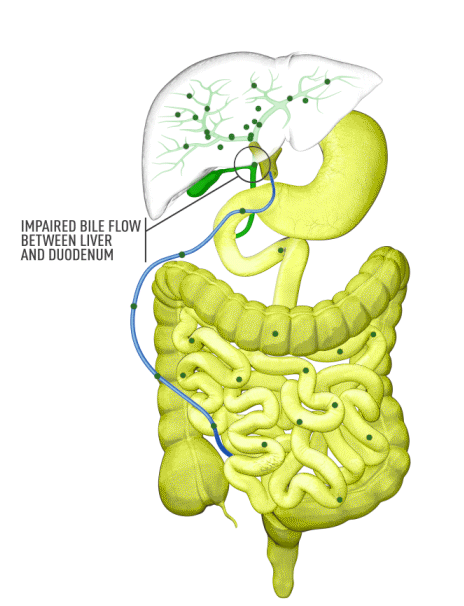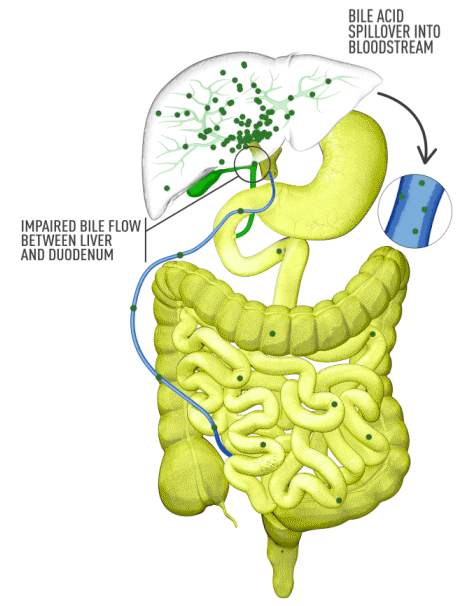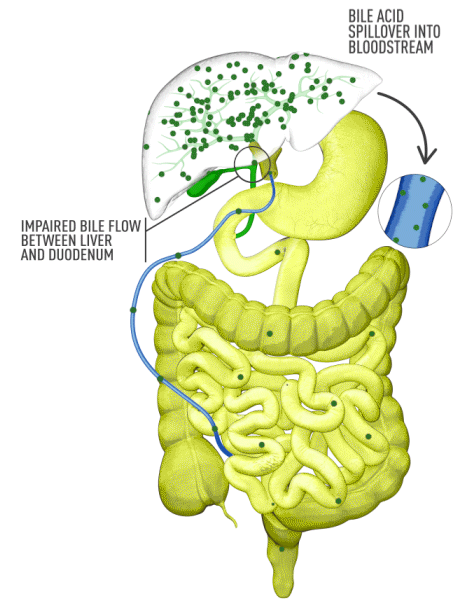
Although the symptoms of cholestatic liver disease may vary based on the etiology, many patients with cholestasis present with intense itchiness, jaundice, dark urine, and pale stools. The impairment of bile flow into the intestine also means that calcium, lipids, and fat-soluble vitamins are poorly absorbed. If cholestasis persists, a deficiency of these nutrients can cause loss of bone tissue.3,4
Chronic cholestatic liver diseases are a significant cause of morbidity and mortality within the pediatric population. The primary cholestatic diseases of infancy and childhood are frequently symptomatic and often rapidly progressive. These chronic cholestatic diseases that present in childhood include biliary atresia, Alagille syndrome, progressive familial intrahepatic cholestasis (PFIC), bile acid synthesis defects, cystic fibrosis-related liver disease, ductal plate abnormalities, primary sclerosing cholangitis (PSC), and certain metabolic diseases.5 This website focuses on Alagille syndrome and PFIC, specifically.
There are several genetic disorders that cause cholestasis, including Alagille syndrome and PFIC. Genetic testing can confirm if a patient is carrying the respective gene and aid in diagnosing patients with these cholestatic syndromes.6 However, there are various investigations that aid in diagnosing cholestatic liver disease.
In Alagille syndrome, variability of clinical presentation and disease severity can result in underdiagnosis, misdiagnosis, or delayed diagnosis. Molecular genetic testing, therefore, provides valuable confirmation, particularly in milder cases or in diagnosis of extended family.7,8
With PFIC, there are several investigations that help to identify its classification into types 1, 2, or 3, and differentiate it from other causes of cholestasis.9 However, no phenotypic features can distinguish PFIC1 from PFIC2. As a result, genetic testing is the only reliable way to distinguish among PFIC subtypes, making it the gold standard in diagnostic tools.9-11
Mirum is proud to sponsor genetic testing through Travere Therapeutics to help with early diagnosis of Alagille syndrome.
The field of inherited cholestatic liver diseases is evolving rapidly as a result of advances in diagnosis based on genetic mutation associations.12
Alagille syndrome is a rare, autosomal dominant, multisystem disorder typically caused by mutations/deletions in the JAG1 gene and/or the NOTCH2 gene.7 Although 30% to 50% of individuals have an inherited pathogenic variant, the mutation occurs de novo in 50% to 70% of cases.13 Mirum is proud to sponsor free genetic testing through Travere Therapeutics to help with early diagnosis.
Alagille syndrome often presents in childhood with a range of clinical manifestations.7 For patients with Alagille syndrome, cholestatic pruritus—an intense, unrelenting itch—is among the most severe in any chronic liver disease, negatively impacting physical health and psychosocial health.7,14
As a result, living with Alagille syndrome can be challenging for patients and their families.
Progressive familial intrahepatic cholestasis (PFIC) is a group of rare, life-threatening autosomal recessive diseases related to functional deficiencies in the hepatocyte transporters.9,11,15 PFIC predominantly affects children, and it has been classified into 3 types—Types 1, 2, and 3—though recent scientific advancements have uncovered a growing list of subtypes that continue to expand our understanding of PFIC. PFIC2, also known as bile salt export pump (BSEP) deficiency, is the most common type.9,10,12,15,16
Cholestatic pruritus has been identified as the most debilitating symptom of PFIC.9 This bothersome pruritus often leads to cutaneous mutilation, loss of sleep, irritability, poor attention, and impaired school performance in children with PFIC.9
With a significant reduction in quality of life, patients and their families face a difficult journey ahead.